|
|
| Sextual Desire Disorders : |
| |
| INTRODUCTION
 The sexual desire and the problems of sexual desire are an area of concern for clinicians since a long time, particularly since mid 1970's. Many authorities have emphasized the psycho-bio nature of the desire phenomenon, that it precedes and accompanies sexual arousal and on the whole generates sexual behaviour. It results from the complex interaction between sexual drive, sexual wish, willingness or aspiration and the sexual motivation. The wish or the aspiration and the motivation are the psychological-cognitive and emotional components while the sexual drive is primarily a biological component, being a neuroendocrine generator of sexual impulses. The force of the drive is generally being accepted as an appetite like hunger or thirst. Like them, the neuro-physiological basis of sexual desire lies in the limbic system. Clinically various degrees of the sexual drive have been recognised. It could be high, moderate, low or absent (Agarwal and Katiyar, 1994). It tends to establish its own level and changes predictably in relation to one's sex, age, nature of up bringing, quality of current relationship and other environmental factors. The sexual desire and the problems of sexual desire are an area of concern for clinicians since a long time, particularly since mid 1970's. Many authorities have emphasized the psycho-bio nature of the desire phenomenon, that it precedes and accompanies sexual arousal and on the whole generates sexual behaviour. It results from the complex interaction between sexual drive, sexual wish, willingness or aspiration and the sexual motivation. The wish or the aspiration and the motivation are the psychological-cognitive and emotional components while the sexual drive is primarily a biological component, being a neuroendocrine generator of sexual impulses. The force of the drive is generally being accepted as an appetite like hunger or thirst. Like them, the neuro-physiological basis of sexual desire lies in the limbic system. Clinically various degrees of the sexual drive have been recognised. It could be high, moderate, low or absent (Agarwal and Katiyar, 1994). It tends to establish its own level and changes predictably in relation to one's sex, age, nature of up bringing, quality of current relationship and other environmental factors.
This manifests as a periodic and spontaneous need for an orgasm. The genital excitement could be recognised by genital tingling, tumescence or lubrication, nocturnal emissions, erotic dreams, partner seeking behaviour, masturbation and erotic fantasies. The wide variation in arousal and excitability is well recognised. Many couples  know the frustration when one feels like having sex while the other would rather turn and sleep. Some people seem to be interested in sex at almost anytime, while others have low or lack of any sexual interest. For the same, since nobody can define a 'normal sex life'. Masters and Johnson insist that desire disorder is present when it leads to marked or significant "personal or relational distress". Having sexual urges, fantasies and activity less than twice a month have been defined as a low sex drive but at best these definitions are quite arbitrary and controversial. know the frustration when one feels like having sex while the other would rather turn and sleep. Some people seem to be interested in sex at almost anytime, while others have low or lack of any sexual interest. For the same, since nobody can define a 'normal sex life'. Masters and Johnson insist that desire disorder is present when it leads to marked or significant "personal or relational distress". Having sexual urges, fantasies and activity less than twice a month have been defined as a low sex drive but at best these definitions are quite arbitrary and controversial.
DEFINITION
The terms like 'Libido', 'Urge', 'Passion', 'Hominess', 'Impulse', 'Need', 'Instinct', etc. have been used interchangeably for desire. However, these terms are more explanatory than descriptive and can create confusion. Hence, it is preferable to use the term 'SEXUAL DESIRE' as such. Levine in his review recognises that despite the concentration of clinical work and writings on sexual desire disorders, hardly any worth while attempt has been made to define it.
The most accepted definition could be that "sexual desire is a psycho-biologic energy that precedes and accompanies arousal and it tends to produce sexual behaviour". It fluctuates in frequency and intensity all through one's life. |
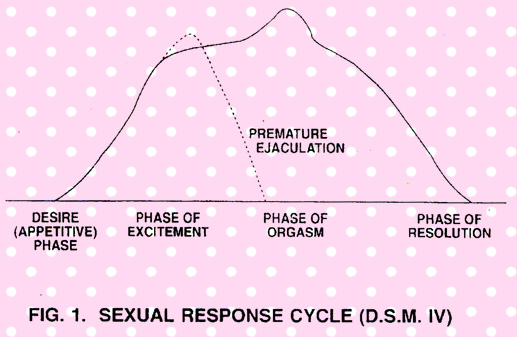 |
The sexual response cycle as reported by Masters and Johnson had recognized 4 phases - excitement, plateau, orgasm and resolution. DSM-IV classification of American Psychiatric Association recognises the Desire or Appetitive phase as a distinct stage in the response cycle (Fig. 1). So also disorders of this stage are explicitly recognised as such. The excitement stage includes both the excitement and plateau phases described by Masters and Johnson. In the desire phase, the emphasis is on various sensory stimuli like visual (by far the strongest), olfactory or tactile and or the fantasies. |
| |
AGE |
FEMALE |
MALE |
| |
|
| Monthly |
| sexual |
| activity (approx) |
|
|
| Monthly |
| sexual |
| activity (approx) |
|
Under 16 |
16-20 |
21-25 |
26-30 |
31-35 |
36-40 |
41-45 |
46-50 |
51-55 |
56-60 |
61-65 |
66-70 |
|
22 |
50 |
72 |
84 |
88 |
89 |
87 |
84 |
77 |
66 |
47 |
37 |
|
|
95 |
99.3 |
99.6 |
99.5 |
99.7 |
99.5 |
99.1 |
97.5 |
96.0 |
95.3 |
81.0 |
73.3 |
|
11 |
11 |
11 |
12 |
11 |
11 |
8 |
7 |
6 |
5 |
3 |
1 |
|
|
* Includes masturbation and intercourse (After Kinsey, et al). |
|
| |
 EPIDEMIOLOGY EPIDEMIOLOGY
Clinically, the individuals or couples may present with little or too much of sexual desire and at present they constitute the most frequently seen sexual problems. Levine opines that many conditions diagnosed as arousal problems in earlier decades are currently viewed as problems in the desire phase of the sexual response cycle.
ICD.10 recognised excessive sexual drive as a condition but it is more a theoretical concept than an actual observation in practice. It is said that a woman with a voracious sexual appetite is a Nymphomaniac while in man it is "Don Juanism". Sexual addiction or sex addiction, a term used by Patric Carnes, is a relative phenomenon and indicates an unhealthy obsession with sex. Much of the research data we have is from western studies. Frank et al (1978) surveyed 100 well educated and married couples and reported that 50% of men and 77% of women had lack of interest in sex and were unable to relax. Nathan (1986) analyzed 22 general population sex surveys to estimate the prevalence rates for various sexual dysfunctions. 1 to 15% of men and 1 to 35% of women had desire disorders, mainly that of reduced sexual desire. Bechtel and Stains (1996) showed that low sexual desire is the main complaint of upto 55% of couples who show up at sex therapy clinics, making it the most common sexual complaint of all. Research has also demonstrated that it is drastically increasing in the last 20 years. This had been attributed to the fact that women's new found liberation and aggressiveness is a turn-off to many men. it is also possible that society and media generated a hype that everybody is having sex and nothing but sex that is frequent. Hence, the social pressure to be a superman and when the ideal is not met, people tend to define it as a problem. In the Indian context a retrospective comparative study of hospital and clinic population of 2 years by the author and colleagues (99) showed desire disorders being significantly higher in females than in males.
 DEVELOPMENT OF SEX DRIVE DEVELOPMENT OF SEX DRIVE
Biologically, sex drive is determined by periodic production of neuro-endocrinal impulses from the limbic systems. This process in both males and females is dependent on the circulating levels of androgens. The hormone primarily responsible for the desire in both the sexes is testosterone. It is known that only 5% of testosterone, which is in free form is physiologically active that the circadian rhythm of testosterone release is such that level is gradually increasing during sleep to reach a maximum towards early morning. Freud believed that girls centered their sexual pleasure in their clitoris during pubertal stage and with maturity they switched it to vagina. Kinsey, Masters and Johnson, Shere Hite and other sex researchers have shown that no such change takes place. Clitoris remains the focus of female libido and is not indicative of any immaturity.
MALE AND FEMALE SEX DRIVE
Research surveys show conclusively that men are more sexually active at all ages than women and that appears to be the case even in the most permissive countries too (Table 1). However, permissive sexual attitudes, availability of reliable contraceptives and relative ease of obtaining legal abortion have brought down the differences to an extent by removing traditional restraints on women's sexuality.
MALE SEX DRIVE
 Men have a stronger overt sex drive and are more open in their desire for sexual contact than women. The important physical and social reasons are as follows : Men have a stronger overt sex drive and are more open in their desire for sexual contact than women. The important physical and social reasons are as follows :
- For men, orgasm and intercourse are inevitably linked. For a man, intercourse invariably leads to orgasm, hence pleasure and therefore he seeks it more frequently.
- It is socially acceptable for men to enjoy and want sex. Men with great sexual prowess as legendary Casanova have become great heroes.
- Men are expected to be lustful and those who show disinterest in the opposite sex are treated with suspicion.
- Upbringing teaches males to be interested in sex - many parents worry about sons who are reluctant to go out with girls, at least in western culture.
FEMALE SEX DRIVE
Female sex drive is less intense than in men. Important reasons are:
-
 Many women find it difficult to achieve orgasm. Rather this appears perfectly normal. In her, achieving orgasm does not come through intercourse alone but is achieved by skilled love making and the stimulation of sensitive areas such as clitoris. Unless a woman has a partner who understands this, for her orgasm is impossible. Therefore, intercourse does not automatically mean intense pleasure to woman as to a man. So- many women do not seek it enthusiastically resulting in lower sex drive. Many women find it difficult to achieve orgasm. Rather this appears perfectly normal. In her, achieving orgasm does not come through intercourse alone but is achieved by skilled love making and the stimulation of sensitive areas such as clitoris. Unless a woman has a partner who understands this, for her orgasm is impossible. Therefore, intercourse does not automatically mean intense pleasure to woman as to a man. So- many women do not seek it enthusiastically resulting in lower sex drive.
- Women suffer less from sexual frustration in diversions like sentimentality, romance, love, etc.
- Girls are actively discouraged interacting with boys, particularly in traditional societies like ours.
- Very few parents teach daughters that sex is a joyous, pleasurable thing. It is taught as a duty, what men need and that women have to tolerate.
- Social attitudes where sensuality in women is invariably branded as 'loose' etc.
-
Physiologically, there is a significant cyclical hormonal fluctuation in women. This results in a variable sexual drive.
CLASSIFICATION OF DESIRE-PHASE DISORDERS
 The decrease in sexual desire is the commonest clinical presentation. Hyperactive sexual desire disorder is primarily of research importance. It is to be emphasized that in the desire-phase disorders the capacity for physical sexual response is usually preserved and the problem is one of lack of willingness to participate in sexual relations due to either fear or lack of interest (Masters and Johnson, 1986). If the lack of interest is the predominant problem, it is classified as Hypoactive sexual desire disorder (Table 2). If the lack of participation is mainly due to overwhelming fear it is referred to as Sexual aversion disorder (Table 3). Like other sexual dysfunctions they could be life long or acquired type. They could be (a) generalized or (b) situation specific i.e. they occur only in a certain context, with a particular partner etc. It could be due to psychological factors or due to combined factors where pathology is invariably multifactorial. Biological factors may be secondary to general medical condition or due to a particular substance abuse.
As gender role discrepancies are well recognized, if sexually active partners consistently describe different appetites for sex and are unable to compromise, Bancroft (1983) labels the problem as sexual dissatisfaction instead of sexual disorder and is diagnosed as 'Desperate levels of sexual interest'. The term ISD is reserved for those situations of abnormally low libido in which an aetiologic diagnosis has been made i.e. when it is established that sexual desire is inhibited by psychic factors. The term HSD is preferable when the aetiology of low libido has not yet been determined. The diagnosis of Hypoactive or inhibited sexual desire disorder is used only when an individual evidences low initiatory behaviour and or a persistently negative receptivity to sexual approaches by an established partner. Frequency of sexual encounter is avoided as a diagnostic standard due to its changes with age and health. Masturbatory behaviour and sexual fantasy are reliable indicators, if at all, only in cases of hypogonadism. The decrease in sexual desire is the commonest clinical presentation. Hyperactive sexual desire disorder is primarily of research importance. It is to be emphasized that in the desire-phase disorders the capacity for physical sexual response is usually preserved and the problem is one of lack of willingness to participate in sexual relations due to either fear or lack of interest (Masters and Johnson, 1986). If the lack of interest is the predominant problem, it is classified as Hypoactive sexual desire disorder (Table 2). If the lack of participation is mainly due to overwhelming fear it is referred to as Sexual aversion disorder (Table 3). Like other sexual dysfunctions they could be life long or acquired type. They could be (a) generalized or (b) situation specific i.e. they occur only in a certain context, with a particular partner etc. It could be due to psychological factors or due to combined factors where pathology is invariably multifactorial. Biological factors may be secondary to general medical condition or due to a particular substance abuse.
As gender role discrepancies are well recognized, if sexually active partners consistently describe different appetites for sex and are unable to compromise, Bancroft (1983) labels the problem as sexual dissatisfaction instead of sexual disorder and is diagnosed as 'Desperate levels of sexual interest'. The term ISD is reserved for those situations of abnormally low libido in which an aetiologic diagnosis has been made i.e. when it is established that sexual desire is inhibited by psychic factors. The term HSD is preferable when the aetiology of low libido has not yet been determined. The diagnosis of Hypoactive or inhibited sexual desire disorder is used only when an individual evidences low initiatory behaviour and or a persistently negative receptivity to sexual approaches by an established partner. Frequency of sexual encounter is avoided as a diagnostic standard due to its changes with age and health. Masturbatory behaviour and sexual fantasy are reliable indicators, if at all, only in cases of hypogonadism.
|
Table 2 : DSM-IV Diagnostic Criteria for Hypoactive Sexual Desire Disorder |
| |
| |
A. Persistently or recurrently deficient (or absent) sexual fantasies and desire for sexual activity. The judgement of deficiency or absence is made by the clinician, taking into account factors that affect sexual functioning, such as age and the context of the person's life.
B. The disturbance causes marked distress or interpersonal difficulty.
C. The sexual dysfunction is not better accounted for by another Axis I disorder (except another sexual dysfunction) and is not due exclusively to the direct physiological effects of a substance (e.g. a drug of abuse, a medication) or a general medical condition. |
| |
|
|
| |
| Table 3: DSM-IV Diagnostic Criteria for Sexual Aversion Disorder |
| |
| |
A. Persistent or recurrent extreme aversion to, and avoidance of, all (or almost all) genital sexual contact with a- sexual partner.
B. The disturbance causes marked distress or interpersonal difficulty.
C The sexual dysfunction is not better accounted for by another Axis 1 disorder (except another sexual Dysfunction) |
| |
|
|
| |
| FACTORS WHICH DECREASE SEX-DRIVE |
| |
A. BIOLOGICAL :
 Decreased testosterone levels. Decreased testosterone levels.- Decreased L.H.R.H.
- Decreased thyroid hormones.
- Increased, prolactin levels.
- General medical conditions like cardiac, renal, respiratory and other chronic, severe illnesses. Other endocrine disorders like diabetes mellitus etc.
- Medications which block dopamine receptors such as anti-psychotics, medicines which elevate serotonin e.g. antidepressants, fluoxetine and others, antihypertensives, mood stabilizers like lithium and other drugs.
- Neuro-psychiatric disorders, in particular depression, obsessive compulsive disorder, epilepsy, Parkinsonism etc.
B. PSYCHOLOGICAL FACTORS :
decreased self esteem, anger, hostility, guilt, anxiety secondary to other sexual dysfunctions, early conditioning, sexual trauma, fear of intimacy or separation, other relational issues like lack of trust, power and control issues, attitudes, religious and cultural beliefs, sexual ignorance and myths, absence of fantasies, distracting thoughts or antifantasy like harbouring fantasies incompatible with sexual arousal.
 FACTORS WHICH INCREASE THE SEX-DRIVE FACTORS WHICH INCREASE THE SEX-DRIVE
- Mania, is the commonest cause
- Alcohol, in the initial stages
- Substances of abuse when used occasionally and in low doses.
- Drugs which enhance dopamine functions such as L-Dopa, bupropion, etc.
- Certain cerebral degenerative disorders, due to disinhibition and in certain types of epilepsies.
Depression is perhaps the most common physiologic cause of HSD. Depression is marked by a diathesis of vegetative symptoms which include sleep, eating and libido disturbances.
Severe stress such as is experienced on the battlefield or during a traumatic divorce or after a job loss is often associated with a loss of sexual interest.
APHRODISIACS
 Aphrodisiacs are substances which are supposed to increase sexual desire. Oysters, powdered rhinoceros horn, Ginseng, animal testicles are a few of the common ones attributed to increase sexual desire. However, there is no established drug or miraculous potion which has such an established effect. At best these are harmless but at worst they can be dangerous. One aphrodisiac known as Spanish fly is a serious irritant which can be very damaging to sensitive urethral tissues. The so called aphrodisiac effect may be because of PLACEBO EFFECT. Aphrodisiacs are substances which are supposed to increase sexual desire. Oysters, powdered rhinoceros horn, Ginseng, animal testicles are a few of the common ones attributed to increase sexual desire. However, there is no established drug or miraculous potion which has such an established effect. At best these are harmless but at worst they can be dangerous. One aphrodisiac known as Spanish fly is a serious irritant which can be very damaging to sensitive urethral tissues. The so called aphrodisiac effect may be because of PLACEBO EFFECT.
The ideas that special foods, drugs or concoctions will arouse libido is a pure fantasy but there are certainly some human factors which increase sex drive. Being in love is the greatest stimulant many couple could ever hope to find.
TREATMENT
Among all the sexual dysfunctions desire disorders are the most difficult to treat.
A. HYPOACTIVE SEXUAL DESIRE DISORDER
- Like sexual dysfunctions in general, many disorders of sexual desire arise because of basic sexual misinformation, lack of experience or destructive relational transactions (Masters and Johnson, 1986). These can be effectively treated by permission giving and educational components of sex therapy. Cognitive behaviour therapy helps alleviate maladaptive beliefs.
- If spectator role and the performance anxieties are the main blocks, brief psychotherapy and behaviour therapies are to be carried out. Exercises to enhance sexual pleasuring like sensate-focus, non-demand sexual stimulation and improving communication are essential.
- In presence of significant intimacy disorder long term psycho-dynamic psycho-therapy is advocated.
- Relational problems need to be attended to by marital therapy.
- Drugs.
a. Testosterone
a.l The effect of testosterone is most dramatic in hypogonadal men. It has been demonstrated that androgen withdrawal results in rapid decrease in sex drive and activity while its replacement restores sex drive and activity to normal (Bancroft and Wu, 1983).
a.2 As one ages, there is a demonstrable decrease in plasma testosterone levels, loss of circadian rhythmicity of testosterone and increase in circulating aestrogens. Hence, it is believed that decreased testosterone levels are the cause of age related decrease in sex desire and activity. Here, testosterone replacement could be beneficial. It must be administered with caution because of its potential effect on the prostate.

a.3 Normally, for the physiological effect, testosterone, has to be converted into dihydrotestosterone and subsequent aromatization to oestradiol. In normal men, circulating androgen levels are far higher than the threshold level required for physiological action. Hence, the endogenous variations or exogenous administration of testosterone does not produce any demonstrable effect in sex drive.
a.4 The androgens maintain sex desire and activity in women. Testosterone in minimal non-masculinizing dosages can be included with good therapeutic effect in post- menopausal women.
a.5 Testosterone has been empirically used to increase libido in
women but its side-effects to be weighed in individual cases.
b. Dopaminergic drugs and other so-called aphrodisiacs may have
secondary desire enhancing effects.
SEXUAL AVERSION DISORDER
Major goal of treatment is to reduce the patient's fear and avoidance of sex. In clinical practice they carry the worst prognosis.
- Systematic desensitization - Patient is gradually exposed in imagination under relaxation and then in-vivo to the actual sexual situations which generate the anxiety.
- Marital therapy to correct relational problems.
- Psychotherapy - Brief and psychodynamic-oriented are beneficial.
- Pharmacotherapy - Tricyclic antidepressants, particularly imipramine and benzodiazepines like Alprazolam are found to be very effective in controlling phobic anxiety.
- Sex therapy using education, permission giving and improving communication is a must in all the cases.
Female Sextual Disorders
DEFINITIONS
 Orgasm is characterised by feelings of heightened excitement, a peaking of subjective pleasure and subsequently release of sexual tension. Orgasm is characterised by feelings of heightened excitement, a peaking of subjective pleasure and subsequently release of sexual tension.
Women's orgasmic contractions may continue longer than those of men. Also, women can experience multiple orgasms in close succession, whereas men cannot. However, women's experiences of orgasm are quite varied.
Orgasm or sexual climax may be produced by stimulation of genital organs e.g. clitoris, vagina.
Orgasmic dysfunction or disorder (OD) refers to those women who are unable to achieve orgasm or have great difficulty in reaching climax in the presence of sufficient sexual stimulation.
Anorgasmia is the term synonymously used to indicate inability of the women to achieve orgasm.This is classified into two types:
 Primary - the woman has never experienced orgasm. Primary - the woman has never experienced orgasm.
Secondary - the disorder has developed after a period of being able to reach orgasm.
It is also classified as:
Absolute - where the woman is unable to achieve orgasm under any
circumstances.
Situational - where she can reach a climax only under specific circumstances. Other synonymous terms used for orgasmic disorders is inhibited female orgasm. Prior to 1970, the term frigid was used to describe the women who did not respond with orgasm when stimulated sexually. Because this term is pejorative, it is no longer used.
AETIOLOGY
Various aetiological factors may be responsible for producing this disorder. They are depicted in the following figure : |
| |
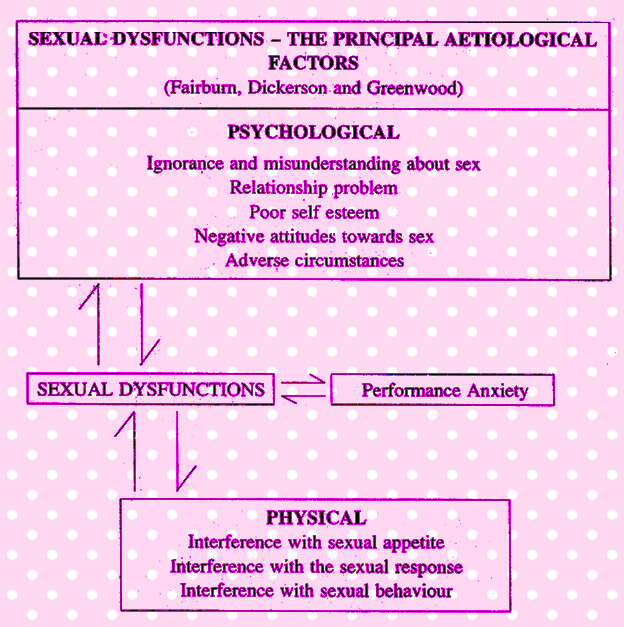 |
 According to Masters and Johnson, about 95% cases are psychogenic in origin. Causes producing vaginismus, may cause OD, conditions that affect the nerve supply to the pelvis or conditions that impair the vascular integrity of vaginal circulation, many endocrine disorders, chronic illnesses can cause loss of orgasmic responsiveness. According to Masters and Johnson, about 95% cases are psychogenic in origin. Causes producing vaginismus, may cause OD, conditions that affect the nerve supply to the pelvis or conditions that impair the vascular integrity of vaginal circulation, many endocrine disorders, chronic illnesses can cause loss of orgasmic responsiveness.
Many of the psychological factors like anxiety, guilt and depression may cause OD. It is important to remember that many women derive considerable pleasure from their sex life without ever experiencing orgasm. Nevertheless, if the woman thinks that she is having undue difficulty reaching orgasm there can be considerable sense of distress.
About one third of diabetic men are impotent. This is a major clinical problem which has naturally received a great deal of attention. Less interest has been taken in sexual function in women with diabetes, because, women seldom complain of sexual problems when they attend a diabetic clinic, Kolodny reported a reduction in the frequency of orgasm in diabetic women. He found total absence of orgasmic response in 35% of diabetic women and only 6% of the control group. Orgasmic problems had developed in most women after the onset of diabetes. The prevalence of sexual dysfunctions showed a distinct relationship with the duration of diabetes, but not with age or the presence of complications. Compared to insulin dependent diabetes mellitus (IDDM), the women with non-insulin dependent diabetes mellitus (NIDDM) have reduced sexual desire; orgasmic capacity, lubrication and sexual activity. It was also found that women with NIDDM have a poor sexual body image.
 Female circumcision is practised in a few African and Asian societies. This may be performed at birth, childhood or at puberty. This is an important cause of OD in these women. Female circumcision is practised in a few African and Asian societies. This may be performed at birth, childhood or at puberty. This is an important cause of OD in these women.
Certain drugs are likely to produce diminished libido, impaired arousal and dryness of vagina, leading to orgasmic dysfunction. These drugs include antihistamines, barbiturates, corticosteroids, some anti-hypertensive drugs and hormone preparations.
INCIDENCE
At any sexual problems clinic, men tend to complain of difficulties with erection or ejaculation, whereas most women complain of inadequate enjoyment. Very few women complain of inadequate lubrication or orgasmic difficulties. Orgasmic disorder is the most prevalent sexual problem among women. Because of differences in the definitions of OD, incidence reports vary. It has been estimated that 8 to 15 per cent of all American women have never experienced orgasm at any time other than during sleep. Situational inhibited female orgasm has been experienced by as many as 50% of all women.  Organic precipitants of OD, such as effects of alcohol, barbiturates and narcotics and inflammatory or infectious conditions are responsible for the problem in less than an estimated 10% of cases. Organic precipitants of OD, such as effects of alcohol, barbiturates and narcotics and inflammatory or infectious conditions are responsible for the problem in less than an estimated 10% of cases.
Kinsey and his colleagues reported that 10% of married women never experienced coital orgasm. Chesser found that 10% of 3705 married British women rarely experienced orgasm, while 5% never experienced orgasm during intercourse.
We do not have statistics regarding the incidence of OD in India. Attendance of female patients either to a sexologist or sexual medicine clinic' itself is very much less compared to males. Most of the consultants who practise sexology exclusively in metropolitan cities are visited by 10-15 new patients per day. Many of the women contact them on phone for advice. Many of popular women's magazines have a column on sexual/personal problems in which problems are answered by the qualified medical persons.
CLINICAL PRESENTATION
A woman rarely complains of OD when she approaches a physician. The woman may have this complaint due to partner's sexual problems like erectile dysfunction or ejaculatory disturbances. A known diabetic patient may be asked  about her sexual activity or responsiveness. A woman with fertility problem may be questioned in detail regarding her sexual satisfaction. Fogel and Lauver suggest following important points to be included in a client's history to establish a diagnosis of orgasmic dysfunction : about her sexual activity or responsiveness. A woman with fertility problem may be questioned in detail regarding her sexual satisfaction. Fogel and Lauver suggest following important points to be included in a client's history to establish a diagnosis of orgasmic dysfunction :
- Contraceptive practices and reproductive goals.
- Is there a fear of pregnancy? Are adequate contraceptive methods being used?
- Is there a desire to be pregnant and is this a share or one sided go?
- Sexual attitudes of both partner.
- Confirmation of whether or not the woman has truly not experienced orgasm is important. Because some women have unrealistic expectations and misinformation regarding orgasm.
- Response to all types of sexual stimulation should be determined; for example masturbation and vibrator use.
- Sexual response with other partners if she had/has any earlier or currently.
- Any homosexual tendency or experiences.
- Whether the woman has/had any psychiatric problem and the effect of its treatment.
Kolodny, Masters and Johnson suggest additional information to be obtained
from the patient regarding her self esteem and body-image.
A detailed physical examination of the patient should be done either in the
presence of the husband or a female attendant. Examination of genital organs helps in clearing the sexual myths of both the partners. They should be encouraged to ask their doubts and fears, so that scientific explanations can be given.
It is always preferable to have the sexual partner/husband for taking cross history. This also helps in getting his co-operation during the courses of therapy subsequently.
These women :
- Have a strong sexual desire
- Enjoy sexual foreplay
- Lubricate copiously
- Love the sensations of phallus penetration
- Have no inhibition of erotic, feelings and
- Show signs of vasocongestion. But they get 'stuck' at or near the plateau phase of sexual response and find no orgasmic relief.
TREATMENT
 Approaches to treatment of the woman with OD must take into consideration
whether it is primary or secondary and the woman has a current sexual partner.
Treatment in all these cases varies, but shows the common element of increasing
self awareness and teaching effective self stimulation. Approaches to treatment of the woman with OD must take into consideration
whether it is primary or secondary and the woman has a current sexual partner.
Treatment in all these cases varies, but shows the common element of increasing
self awareness and teaching effective self stimulation.
Misconceptions regarding sexuality require correction. Similarly vascular,
neurological or psychological factors need attention. If the endocrine disorders
like diabetes are found they should be accordingly managed.
Anatomical and physiological aspects of sexual response cycle should be discussed with the couple. In case of primary OD masturbation training and progress to sensate focus exercises with the partner is advocated. In some cases, duration of masturbation may be increased to 30-45 minutes. Regarding erotic material and fantasizing during masturbation can also be helpful. If no orgasm occurs the woman can try using a vibrator like the one used for facial massage. The woman with secondary orgasmic dysfunction, the problem is usually one of decreased frequency of coital orgasm. Masturbation training may help to re¬establish higher degree of sensitivity, to pleasurable sensations, clarify what is indeed most stimulating to the woman and establish the effectiveness of self-stimulation or genital manipulation during coitus.
Sensate focus exercises are advocated by Masters and Johnson for all sexual problems including orgasmic dysfunction. In this method of treatment, therapists teach, guide and instruct the couple. All actual sexual activity is carried out by the couple alone privately in their own bedroom. The therapists should not watch or film the couple. They should not have sexual relations of any  kind with their clients. kind with their clients.
Various types of behaviour therapies are found effective in treating orgasmic dysfunction. These include shaping, systematic desensitization and PLISSIT. Anon felt that all patients do not require elaborate sex-therapy or psychotherapy. He advocated PLISSIT approach; that is four levels of treatment consisting of: Permission
Limited information
Specific suggestions
Intensive therapy
He feels that the first two or three levels of therapy are sufficient in many sexual problems including orgasmic dysfunctions. Intensive therapy may be required in very few cases and should be carried out by a qualified sexologist.
IN OUR EXPERIENCE
Hypnotherapy is another method of treatment of sexual disorders including
orgasmic dysfunction. In this therapy positive suitable suggestions depending
upon the patient's problems are given during the trance state to her. The treatment
requires 10-15 sessions over a period of 8-10 weeks. Various grades of
improvement were found in 50% of patients.
Medical disorders like diabetes, hypertension and anaemia require appropriate
treatment. Similarly gynaecological and surgical conditions should be treated
simultaneously.
|
| |
|
| |
|